I want to help you manage your type 2 diabetes naturally. Controls For Diabetes may collect a share of sales or compensation from the links on this page.
What Does Insulin Resistance Mean?
 Fewer people smoke, people are living longer, and we have the latest state of the art medical treatment for heart disease, stroke, and cancer. Can you believe people are still unhealthy, and overweight? 80 percent of type 2 diabetics are overweight, and type 2 diabetes is past epidemic proportions. Obesity, insulin resistance and type 2 diabetes are they related? What does insulin resistance mean?
Fewer people smoke, people are living longer, and we have the latest state of the art medical treatment for heart disease, stroke, and cancer. Can you believe people are still unhealthy, and overweight? 80 percent of type 2 diabetics are overweight, and type 2 diabetes is past epidemic proportions. Obesity, insulin resistance and type 2 diabetes are they related? What does insulin resistance mean?
In 1971
Insulin receptors are discovered on cell membranes. This discovery raises the possibility that missing or defective insulin receptors may prevent glucose from entering the cells. Thus contributing to the insulin resistance of type 2 diabetes. From the history of the American Diabetes Association.
Fast forward to 2017
Even though medicine is so advanced, people do not look like they did before. Do not feel as good, and are suffering from serious medical problems. People have different shapes than before, bigger bellies, and bigger abdomens. They are obese. (Obesity means being at least 20 percent over the ideal body weight for one’s height, build, and sex.). Thin people have potbellies. Obesity is out of control! The cause is the hormone insulin.
Discovery of insulin
Fredrick Banting, Charles Best, and John Macleod discovered insulin at the University of Toronto in 1921. They first tested on dogs, successfully. Needing more insulin, they used cows. In late 1921 a biochemist Bertram Collip, joined the team, who purified the cows insulin for human use. In January of 1922 they injected Leonard Thompson a young 14 year old, with type 1 diabetes.
The test was a success, otherwise he was near death and would surely have died. Type 1 diabetes before 1922 was a death sentence. He regained his strength and appetite, then went on to live another 13 years.
Later on they tested the insulin on other diabetics with the same success. In 1923 the Nobel Committee awarded Banting and Macleod the Nobel Prize in Physiology or Medicine[1]. Type 1 diabetes was a fatal disease due to diabetic ketoacidosis (DKA), a buildup of acids in the blood. Blood sugar is very high and the cells cannot convert into energy due to a severe lack of insulin.
Instead fats in the body will be burned for fuel. Burning the fats produces acid called ketones, if there is no insulin this process will go on and build up in the blood. High amounts of ketones will be excreted with glucose in the urine. Weight loss and the chemical balance of your entire system will collapse. You will become very ill, very quick.
Symptoms include confusion, rapid breathing, abdominal pain, a fruity smell to one’s breath, and or go into a coma. Insulin must be is administered, or death is imminent. Type 1 diabetes is now a chronic disease treated with insulin.
What is Insulin?
Let’s start at the pancreas, a large gland about the size of your hand, located below the stomach behind the abdominal cavity. It is responsible for manufacturing, storing, and releasing the hormone insulin. The pancreas also makes several other hormones, as well as digestive enzymes naturally. We all have to have insulin to survive.
Insulin is a hormone produced by the beta cells of the pancreas. The main function is to regulate the level of glucose in the blood stream. By facilitating the transport of blood glucose into all of the billions of cells in the body.
Insulin stimulates glucose transporters to move to the surface of cells to allow glucose entry into the cells. Like a key unlocking a lock. Insulin also stimulates centers in the hypothalamus of the brain responsible for hunger and satiety. As we begin to eat insulin secretes before glucose hits the bloodstream.
Insulin also instructs fat cells to convert glucose and fatty acids from the blood into fat. The fat cells then store until needed. Insulin is an anabolic hormone. It is essential for the growth of many tissues and organs. In excess, it can cause excessive growth, for example, of body fat and of cells that line blood vessels.
Finally, insulin helps to regulate, or counter-regulates, the balance of certain other hormones in the body.
Insulin As A Storage
When you eat, processed foods/carbohydrates/proteins the pancreas secretes the hormone insulin. To help move the sugar (glucose) into your cells, where it’s used for energy. Glucose and sugar will be used interchangeably. Excess glucose is either stored in the liver as glycogen where it will be used later as the body needs it, or turns it into fat.
The liver has limited space and has room for a limited amount of glycogen. Any excess glucose is turned into fat by a process called De Novo Lipogenesis (DNL). Which means “to make new fat.”
Insulin tells the excess glucose to be stored as new fat, called triglyceride molecules. The fat is exported out of the liver to be stored in fat cells later supplying the body when needed. Insulin provides the signal to stop burning glucose and fat, resulting in storage.
Glycogenolysis, takes the glucose from glycogen and will send the glucose to parts of the body where energy is needed. So when feeding and insulin is high there is a balance, when fasting and insulin is low, the result is no weight gain. The result is a metabolically healthy system and provides glucose for short term fasting, up to 36 hours.
Gluconeogenesis is the opposite of the glycogen process and will take the stored fat in the liver in times of prolonged fasting and not eating.
Another factor of insulin, when the liver has a full limited supply of glycogen, there will not be room for DNL. These triglyceride molecules are packaged together with specialized proteins, called lipoproteins, which are made in the liver and exported into the bloodstream as Very Low-Density Lipoprotein (VLDL).
Insulin activates the hormone LipoProtein Lipase (LPL), which signals fat cells, called adipocytes. The adipocytes remove the triglycerides from the blood for storage as body fat.
Excess Glucose
On the other hand, if the body cannot burn off the excess glucose, the pancreas secretes even more insulin to overcome this resistance. This forces more glucose into the overflowing cells to keep blood levels normal. The effect is temporary as there is still excess glucose. As a result, it has moved the excess from the blood to the cells, making more insulin.
Insulin Resistance
Even though insulin is still secreting, the insulin cannot force anymore glucose into the cells. We then say that the body has become insulin resistant, insulin does not know any better. It is a hormone reacting the way it should. The primary problem is that the cells are overflowing with glucose. The insulin resistance cycle continues until it reaches a stage of too much glucose. There are many metabolic problems that may develop along the way.
If you don’t burn off that glucose, then over a long period, it could be years or decades. Cells become filled and cannot handle anymore. The next time you eat sugar, insulin cannot force anymore glucose into the filled cells. It has nowhere to go, so the excess stays in the blood. When there’s too much glucose in the blood, insulin does not appear to be doing its job of moving the sugar into the cells.
The high blood glucose is only part of the issue. Not only is there too much glucose in the blood, there’s too much glucose in all of the cells. Too much glucose leads to prediabetes and then type 2 diabetes. Kids as young as 3 years old are developing type 2 diabetes, so the insulin resistance cycle is now elevated at months rather than years.
Jason Fung says that he can make you fat by prescribing insulin. Excessive insulin causes weight gain and obesity[2].
Excessive Insulin Drives Obesity
Constantly eating and snacking will result in your insulin secretion predominating over your recover period. The myth of eating 6 times a day will not allow you to fast. This means that the insulin dominance leads to fat accumulation. Too much insulin means more new fat via DNL.
Normally, if the feeding periods of high insulin balance the periods of low insulin (fasting), there should be harmony, weight remains stable. High insulin tells the body to store food energy as body fat. Eating and not allowing the body to recover from insulin will never allow you to be thin.
Our hormones, mostly insulin, ultimately set our body weight and level of body fat. Remember, obesity is a hormonal imbalance, not a caloric one. Says Jason Fung taken from his book The Diabetes Code.
It is a known fact that if people are given insulin and or cortisol they will gain weight. When stopped they lose weight.
Carbohydrate-Insulin Model of Obesity (CIM)
According to Dr. David Ludwig the Carbohydrate-Insulin Model of Obesity (CIM), the following are true and drive weight gain.
1. Processed carbohydrates — think white bread, white rice, potato products, low -fat snacks — raise insulin more than any other food, calorie for calorie. This is just Nutrition, 101.
2. Insulin is the Miracle-Gro for your fat cells. A child with new onset type 1 diabetes — unable to make enough insulin — will invariably lose weight until receiving treatment, no matter how many calories consumed. Give that child the right amount of insulin, and weight trajectory returns to normal. Give that child (or an adult with type 2 diabetes) too much insulin and excessive weight gain will predictably result. This is just Endocrinology 101.
3. When too many of the calories we eat get locked away in fat cells, there aren’t enough calories to supply the needs of the brain and other organs. So we get hungry and “overeat.” And to make matters worse, metabolism slows down, further fueling weight gain. This is just Obesity 101[3].
There is a bit more information that needs to be studied and incomplete according this study[4]. The 3 points are the basis for the CIM but there are other factors that contribute to the model. These factors include medication, drugs, stress, smoking, lack of sleep and much more.
Drug Resistance (Tolerance)
Insulin resistance has the exact same analogy as any other resistance or tolerance.
When cocaine is taken for the first time, there is an overwhelming reaction of the “high.” With each use of the cocaine, this high decreases progressively. The users may increase the dose to achieve the same high. Repeated use and prolonged exposure, will develop resistance to the drug’s effects, this is a condition called tolerance (resistance). People build up resistance to many types of drugs, including heroin, marijuana, nicotine, caffeine, and alcohol. Constant use builds resistance.
Removing the drug removes the resistance. Stop drinking alcohol for a long period, say for a year, the first drink afterwards will have its full effect again.
The term insulin resistance has been around since the seventies. Doctors should be able to diagnosis and treat it if they know what to do. The world is experiencing an epidemic of insulin resistance. A third or more of the American population develops it by the time they turn forty.
Kids, teens and young adults have insulin resistance. The reason is due to the sodas and energy drinks available everywhere. Insulin resistance is now a precursor to type 2 diabetes.
Our Ancestors
People of yesterday had no problems with insulin resistance because they did not eat the processed, refined carbs that we consume today. Diets, workout at the gym and medication are not needed. You need to reduce the amount of insulin your body produces. If you understand this, it should be a piece of cake, pardon the pun.
Now is a good time to get a bloodwork done and the only person who is in control of that is you. Get it done and out of the way. If you have had it done, you know what your A1c is, and then you can monitor your fasting glucose on a daily basis.
People nowadays eat too much starch, sugar and processed refined carbs; hundreds of times more glucose than our prehistoric ancestors did. Our ancestors did not have diabetes because they did not eat process refined carbs.
Some people are the few lucky ones, the others do not handle high glucose so well. The result is obesity, insulin resistance, and many other metabolic complications.
High levels of insulin in the blood down-regulate the affinity for insulin that insulin receptors all over the body have naturally. This “tolerance” to insulin causes even greater insulin resistance.
Banting Lecture
In his American Diabetes Association Banting lecture in 1988, Gerald Reaven used the term “Syndrome X” to describe the relationship of insulin resistance, hypertension, type 2 diabetes and cardiovascular diseases. Insulin resistance is such a high predictor of age related diseases[5].
Known as Reaven’s Syndrome, Syndrome X, Dysmetabolic Syndrome, Multiple Metabolic Syndrome, Diabesity, Metabolic Syndrome X, Metabolic Mayhem, Cardiometabolic Syndrome, Visceral Obesity Syndrome, Prediabetes, and Insulin Resistance Syndrome. Call it whatever you want they all mean the same thing.
Metabolic Syndrome
Untreated Metabolic Syndrome can increase the risk factors to many chronic illnesses. We now know that eating processed foods (for example sodas, sweets, pastas, and breads) can raise glucose, triglyceride and insulin levels. Also, elevated insulin can promote obesity and high blood pressure. The problems are related and occur in clusters, as a result form a syndrome.
Metabolic Syndrome is a disorder that can affect anyone, young, old, and can remain hidden for years, even decades. The symptoms include fatigue, poor mental concentration, abdominal
(apple-shaped) obesity, inflammation, nerve damage and a craving for sugary carbs.
Metabolic Syndrome is defined as the presence of any three of the following:
1. Low HDL Good Cholestrol HDL-C < 40 mg/dl – 1.03 mmol/L in men, < 50 mg/dl – 1.29 mmol/L in women.
2. High Blood Triglycerides TG > 150 mg/dl – 169 mmol/L
3. Abdominal obesity visceral (Large waist size) BMI > 30 kg/m2
4. Hypertension systolic blood pressure > 130 and or diastolic > 85 mm HG
5. Impaired fasting glucose > 110 mg/dl – 6.11 mmol/L
Measure Insulin Resistance
Insulin resistance can be measured only after a blood workup. The best way to measure insulin resistance is through the HOMA-IR test.
The National Cholestrol Educational Program defines Insulin Resistance as the following:
TG > 150 mg/dl HDL-C < 40 mg/dl
BMI > 25 Glucose > 110 mg/dl
Visceral Obesity
The culprit is a particular kind of body fat. Visceral obesity is a type of obesity in which a special kind of fat is concentrated around the middle of the body. Particularly surrounding the organs for example the liver. Males who are viscerally obese have a waist of greater circumference than the hips.
Females who are viscerally obese will have a waist at least 80 percent as big around as her hips. All obese individuals and especially those with visceral obesity are insulin resistant. The ones who eventually become diabetic are those who cannot make enough extra insulin to keep their blood sugars normal.
Body Mass Index – BMI
Is a measure of a persons weight in relation to his or her height.
Calculate using either of these formulas
BMI = weight in kilograms/height in meters squared or BMI = (weight in pounds x 703)/height in inches squared.
Another method of checking obesity is to measure fat at the belly button. How does it look?
How much can you pinch? Can you pinch an inch?
Type 2 diabetes risk may be incrementally higher in those with a higher BMI.
The US department of health considers a person with an index of :
- 19 to 24.9 Normal
- 25 to 29 Overweight
- 30 to 39 Obese
- 40 + Morbidly Obese
Joseph R Kraft
 I stumbled across this fantastic book “The Diabetes Epidemic and You” by Dr. Joseph R Kraft[6]. He was the pioneer of the insulin assay and decoded hyperinsulinemia. Dr. Kraft measured people for Insulin/Diabetic issues. 14,384 people ranging from 3 to 91, for 20 years.
I stumbled across this fantastic book “The Diabetes Epidemic and You” by Dr. Joseph R Kraft[6]. He was the pioneer of the insulin assay and decoded hyperinsulinemia. Dr. Kraft measured people for Insulin/Diabetic issues. 14,384 people ranging from 3 to 91, for 20 years.
Testing was based on an oral glucose tolerance testing (OGTT), glucose is measured in response to drinking glucose. This response identifies how much the body metabolizes and removes glucose from the blood. Important information for diabetes and other metabolic issues.
Dr. Kraft’s tests were different and thorough. First, rather than monitoring glucose for 2 hours, he would monitor for at least 4 and 5 hours. Second, he measured insulin, as well as glucose, over the entire test. Hyperinsulinemia means the same as insulin resistance.
He accurately quantified Type 2 Diabetes in each person. Surprisingly, the prevalence was far higher than perceived from standard tests. He measured their Insulin response to a glucose load, and noticed that there were 5 different patterns of response.
Kraft Patterns
The first group ‘Pattern 1’ is healthy or ‘Euinsulin’ a small percentage were in this group. Within the first hour the insulin will peak and it is back to the baseline, 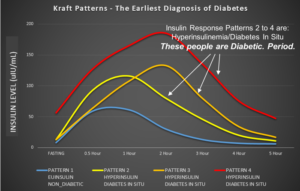 normal pattern. The next Pattern 2, shows insulin resistance and would be overlooked if you just looked at glucose dropping off.
normal pattern. The next Pattern 2, shows insulin resistance and would be overlooked if you just looked at glucose dropping off.
Patterns 3 and 4 show different levels of insulin resistance. Patterns 2 – 4 mean that you are diabetic, his term called ‘Diabetes In-Situ’. Diabetes In-Situ means normal glucose response to abnormal insulin response. My thanks to Ivor Cummins for the diagram.
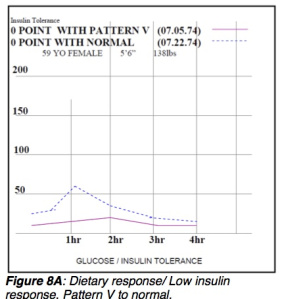 Pattern V could be type 1 diabetes, is a beta cell failure in the pancreas and cannot generate insulin. Another possibility is a healthy person on a low carb diet. The diagnosis in this case is left to the experts.
Pattern V could be type 1 diabetes, is a beta cell failure in the pancreas and cannot generate insulin. Another possibility is a healthy person on a low carb diet. The diagnosis in this case is left to the experts.
Dr. Kraft through his pathology and observations, summarized that:
1. Diabetes can be detected earlier.
2. Abnormally high insulin levels damage the vascular system, and affect every organ in the body.
3. Hyperinsulinemia is a condition and the causal mechanism behind metabolic and chronic diseases.
Once the medical establishment standardizes the test, it would benefit everyone.
I highly recommend you read his book.
How to Reduce Insulin Resistance
1. Reduce added sugar, eliminate desert, if you have to have desert eat nuts, apples, dark natural chocolate (not milk chocolate).
Do not replace sugar with artificial sweeteners, sugar additives, agave or anything similar. No snacking, surprisingly you will save money.
2. Reduce consumption of refined grains, white flour, refined carbs, pasta, and concentrated grain. Eat carbs in the whole natural state. Processed foods increase blood glucose very quickly along with insulin. Follow the Low Carb High Fat diet this is a natural and healthy way of eating
3. Moderate protein in your diet to 20 to 30 % of total calorie intake. No protein shakes, protein bars, protein supplements and processed anything.
4. Increase consumption of natural fats, for example butter, olive oil, coconut oil, nuts, full fat dairy whipping cream, and avocados.
5. Increase consumption of fiber – nuts, natural whole foods, beans, chia seeds, avocadoes, egg plant, and apples.
6. Timing is everything. Eat and fast, try to fast for 20 – 24 hours 2 days a week and 14 to 18 hours for 5 days. You will find that fasting burns fats, lowers blood glucose and normalizes insulin.
7. Try to get 7 to 8 hours of sleep everyday, doing so will keep the cortisol levels in check to reduce blood glucose and insulin.
8. Stop consuming alcohol, drugs and smoking in order to reduce insulin secretion.
Finally
Following these points will give you a better chance with insulin resistance. Consult your doctor or health practitioner before making any change(s) to your lifestyle.
Have a look at these videos and then you can answer my questions.
Video by The Fat Emperor Ivor Cummins – ‘The Pathways of Insulin Resistance: Exposure and Implications‘ .
Video by Dr. Hallberg – Carbohydrate Intolerance, Insulin Resistance and Reversing Diabetes .
Do you understand the meaning of insulin resistance? What does insulin resistance mean? Should you be checked?
I welcome and appreciate any comments, questions or concerns. Please send me an email.
Many thanks for dropping by and reading this post.
References
1. august-krogh-and-the-nobel-prize-to-banting-and-macleod
2. The Diabetes Code: Prevent and Reverse Type 2 Diabetes Naturally, Jason Fung, Greystone Books, 2018. p47.
4. https://www.ncbi.nlm.nih.gov/pubmed/28074888
5. https://www.ncbi.nlm.nih.gov/pubmed/11502781
6. Diabetes Epidemic and You, Joseph R Kraft, Trafford Publishing, 2008.
Recommended Reading (See also Recommended Books To Read)
The Diabetes Code: Prevent and Reverse Type 2 Diabetes Naturally, Jason Fung, Greystone Books, 2018.
Diabetes Epidemic and You, Joseph R Kraft, Trafford Publishing, 2008.

Wow, It is quite exhaustive on the matter “What Does Insulin Resistance Mean”. The knowledge of how insulin overwhelms the pancreas or ‘underwhelms’. It affects the production of sugar that is needed in the right amount in the body as always around the clock any imbalance produces DNL and insulin doesn’t know any better which complicates the matter, insulin is always high which causes fat storage.
The metabolic system is affected. The best cure is to stop eating and fast, 8, 10, or 12 hours a day is an outstanding tip because I only sleep 4 hours a day and I feel fine. However, I realized that just because I feel fine it doesn’t mean I’m ok.
I believe it is the lifestyle. Exercise, proper food, complete rest no refined processed food, and no junk food. Do not eat all the time. We need to do some fasting at some point. That’s a lot of information including avoiding sugar. The best things are the remedies and practical suggestions. Great content.
Hello Florentino,
You seem to have insulin figured out. Only 4 hours of sleep a day is an amazingly low amount of sleep, I don’t know how you do it.
On another note, you should go to your doctor and get a blood panel to make sure your insulin sensitivity is normal. Then when you have your numbers from the test, use the link to the HOMA-IR calculator on my post, let me know if you have any issues.
Thanks for dropping by and your comments.
Jimmy.
Wow, thank you for such an informative article. I had no idea what insulin resistance really was until I read it.
I’m surprised with the don’t replace sugar with alternatives recommendation. I drink a lot of Diet Coke… I guess I should curb that habit.
I do love my carbs but I just started a low carb diet so I guess I’ll be addressing that as I go too.
I’m 43 years old, 5’11” and weigh 208 pounds. I know I’m overweight and although I’m not diabetic yet, it runs in my family so this is a big concern for me.
Thanks again. I’ll be reading this post once more and making sure I have it all figured out in my head and make a decision on how to proceed, mainly with my diet going forward.
Scott
Hello Scott,
I am glad you found the article informative. I estimate there are 2 billion people in the world that are insulin resistant and if you read between the lines it means they are diabetic.
You need too stop drinking diet coke and start drinking tea, or coffee, unsweetened, and of course water.
Find out your carb tolerance, talk to your doctor by getting a blood panel and get the following tests: ALT, fasting glucose, fasting insulin, triglycerides and HDL along with other blood tests that your doctor recommends.
The key is to figure out your insulin and control your insulin sensitivity.
Have a look at the bottom of the page I absolutely recommend you read those books plus another book called “The Blood Code by Dr. Richard Maurer. You can also check out my Recommended Book To Read page you will have months and months of reading.
Let me know if you have any other metabolic issues you need help with.
Thanks for dropping by and your comments.
Jimmy.
Hello Jimmy, you seem to have a very broad knowledge on the discourse topic coupled with the fact that you must’ve done a wide array of research to complement what you already know. I am here also to make a research for an assignment on effects of insulin and your post has been of great value to me. I just wanted to say thank you.
Hello Henderson,
Appreciate the kind words.
I am/was a type 2 diabetic that was misled by my doctor and no offense against him as he is not a metabolic specialist. He is a doctor who like 99 % of the doctors work with big Pharma and prescribe medicine whether it works or not.
I like my doctor because he works out everyday and is slim, I explain to him which tests I need and also tell him which books he should read. He listens, takes notes and tells his clients to check out my website.
As soon as he figures out that the solution to chronic diseases is food and not drugs then I can start asking for his advice.
Prescription drugs are so destructive they end up causing more damage than they cure. Perfect example is Metformin a drug used to lower blood sugar, yes it lowers blood sugar, great, but it does not address the problem of insulin resistance. Other issues from Metformin are nausea, diarrhea, and not feeling well.
Figure out your insulin and you can master your health. Start with a nutritious low carb high fat diet and get off of the Standard Western Diet (SAD).
Check out my Recommended Books To Read page and read: Metabolic Autophagy, Diabetes Epidemic and You, The Blood Code, Food is Your Best Medicine, and The Art and Science of Low Carbohydrate Performance.
Thanks for dropping by and your comments.
Jimmy.
This is a serious subject, that needs careful study, and then some positive action.
I have several family members, who have suffered from this problem, and two who have died.
My brother uses the Banting diet, to avoid taking insulin, and has good success with it.
That type 1 diabetes is very serious I knew, but that it can be fatal, I only discovered while reading this treatise.
It is surprising that with the size of the diabetes problem, and it,s rapid growth, that it is not brought to the public,s notice more widely,and forcefully.
Hello Robert,
I agree with you insulin resistance is a serious subject that needs attention. We know that you must have a nutritious diet and reduce other factors that will lead to insulin secretion.
Any diet that reduces sugar and processed foods should work.
Type 1 diabetes is a chronic condition that can be controlled through exogenous insulin.
I agree we need to spread the word that you must be aware of metabolic issues and you need to start by eating whole unprocessed natural food.
Stay healthy and thank you for commenting.
Thanks for writing this article I really find it so useful and I know many will find it useful to the matter patterning to healthy issue like type 2 diabetes.
Like I always say in cases of diabetes, most of the cause of type 2 diabetes are due to the lifestyle in our day to day activities in what we consume as human being. it is essential to stay away from substance that can have negative effects in our body at a later stage in life. The effect may not be visible now but surely the effect will be visible later. Better to stay away because prevention is better than any cure, meanwhile diabetes has no cure. The only cure is to live a healthy lifestyle
Hello,
I am glad you appreciate and find the information useful.
I agree with you, eat whole natural unprocessed food and you will remain healthy, at least diet wise. Other factors that contribute to insulin resistance are stress, medication, drug use and lack of sleep.
Take care of yourself and you can put type 2 diabetes into remission, it is hard work but can be done.
Stay healthy.
Thanks for your comments.
This is lovely and commendable. Even though as a science student, no one has explained this the way your post has done. I have a better grasp on the subject. I have a Medical doctor friend that eats sugar like no man business, and I got to know from him that sugar is not responsible for type 2 diabetes. Your post clearly confirm this, it is the failure of the body cells to absorb the glucose produced by the insulin that leads to pre-diabetes, and ultimately to diabetes. can exercise help in this regard.?
Hello,
I am glad you appreciate my information.
Your medical doctor friend will eventually experience insulin resistance and full blown types 2 diabetes unless he slows down eating sugar. You should educate your doctor friend and spread the word on a nutritious diet.
I ultimately suggest to everyone and anyone, stop eating sugar and processed foods. An exercise routine is a big factor to lower insulin sensitivity.
Thanks for commenting.
Jimmy.
Hi there. This post is simply educating. I found it hard to understand how diabetes occurs in the human body until now. After reading your explanation I get it.
I have always known that we need insulin to survive but never knew it had been produced by the pancreas.
The insulin resistance is what always leads to some metabolic issue?
I really understand the part that excessive insulin leads to obesity because of excessive sugar.
Thank you for sharing this information
Hello Kehinde,
I am glad that you now understand insulin resistance and that you have been educated by my post.
Insulin as you know plays a vital role in human life, we absolutely need it to metabolize glucose. Not being able to produce insulin will turn you into a type 1 diabetic and you would need exogenous insulin to survive.
Insulin resistance is the root cause of many metabolic conditions, and chronic diseases. A person could be metabolically healthy obese, but for how long? Letting a condition like this go unchecked and you are playing with fire .
Sugar is known as sweet poison, stay away from sugar and processed food.
Appreciate you reading my post.
Thank you for comments.
Jimmy.
It makes so much sense that ancient people did not have problems with insulin resistance and it is purely a disease for recent era because of availability of all those processed food and fake foods (and sugar). It also makes sense that you can reduce insulin resistance by getting rid of those sugary food from your diet coupled with balanced diet. I think schools should teach kids about all this so that they will be making educated decisions as they grow up. Thank you for an informational article.
Hello Saori,
Insulin resistance and type 2 diabetes is also known as processed food disease. I remember Dr. Robert Lustig saying that before and he is absolutely right.
Big Sugar is cashing in on people that are addicted to sugar. Unfortunate, and so sad.
I agree that schools should teach kids about proper nutrition this may reduce the metabolic issues that is so prevalent nowadays.
Thank you for commenting.
Jimmy.
Hi Jimmy, based on research 80 percent of type 2 diabetics are overweight, and type 2 diabetes is past epidemic proportions.
I didn’t know that the excess sugar/carbs starts to build up and causes fats to accumulate and starts the insulin resistance condition which leads to type 2 diabetes.
Reading your article just enlighten my knowledge on how to control diabetes.
Hello Adisa,
Surprisingly people can be metabolically healthy obese, but could be on the edge of insulin resistance and they would fit into the 20 percent range.
Proper diet and nutrition is the key factor to leading a healthy life. Eating processed foods and sugar can take years even decades to go from insulin resistance into full blown type 2 diabetes.
The process is much quicker for kids because of the huge sodas that they consume. Months, kids as young as 3 years old are becoming diabetic.
I am glad that you are enlightened with knowledge on diabetes.
Thank you for commenting.
Jimmy.
Hi ,
I didn’t know how diabetes occurred in the human body. I understand now as you explain, it is the build up of insulin resistance. My mother is suffering from diabetes .
I didn’t know that the excess sugar/carbs starts to build up and causes fats to accumulate and starts the insulin resistance condition which leads to type 2 diabetes.
The insulin resistance problem can be solved by maintaining a nutritious diet and exercise which will prevent the storage of fat in the body .
Thanks for making us aware .
Hello,
I am glad that you understand the insulin resistance condition. I am sorry that your mother is suffering from diabetes. I hope that she can clean up her diet by eating nutritious food and eliminating sugar and processed foods.
Exercising would really help this condition too, start by walking for 5 minutes and build up to an hour per day.
Type 2 diabetes is a processed food disease and can be fixed by eating nutritious food.
Please make your mother and anyone you know aware of the negative affects of processed food.
Thanks for dropping by and commenting.
Jimmy.
HI, I read your whole article – “what does Insulin resistance mean?” In my knowledge insulin increases the immunity of the body.
My parents have diabetes, they also use insulin. I saw the use of insulin after 20 years, it has increased gradually. After reading this, I learned something new.
Thank you so much for sharing this.
Hello,
I am glad you read the article and have an understanding of insulin resistance. As you know once you are insulin resistant you body starts to break down and you become vulnerable to all sorts of chronic and metabolic issues.
For people that are type 2 diabetic like your parents they need to adjust their lifestyle and get off of all medications and insulin. Read my other posts and pages for more information.
Thanks for dropping by and commenting.
Hi Jimmy,
Thanks for writing this awesome educational and informational article. I was impressed by reading this article. If I did not read this article I could not find details about Insulin Resistance. The relationship between insulin and diabetes is quite similar to the heat and temperature relationship.
Insulin is a hormone that is released from the beta cells of the pancreas in the Islets of Langerhans, carbs, protein and other factors will trigger insulin to be released
Insulin resistance is a physical condition where insulin is made in the body, but does not work properly. If a person has insulin resistance, metabolic issues may develop.
Two members of my family have diabetes problems. I am going to share this article with them. My dad likes fast food, so he cannot leave fast food even after we say no more.
Can you tell me to stop him from this? My parents have diabetes but I do not have diabetes yet.
Can I be affected later? I’ve bookmarked this article and I’ll definitely share it with my family and friends.
Hello,
I am glad you appreciate this post, and make an analogy of insulin and diabetes to heat and temperature. OK.
You seem to have grasped the insulin resistance condition, by passing this on to your family members you could definitely help them with their metabolic issues.
I can definitely tell you to stop him, but he has to do that on his own. Your father has to change his mindset and want to change his lifestyle. Once you do that then you can start eating healthily, exercising, walk for an hour a day, and get 7 to 8 hours of sleep.
Can you be affected by insulin resistance? Yes, anyone can be affected. Start by changing your lifestyle as I mentioned above. I suggest you check out my posts and pages. Specifically Low Carb High Fat diet and Intermittent Fasting.
Thanks for dropping by and commenting.
Jimmy.
Hi Jimmy.
I liked reading your post. Clear, easy to read and understand.
For me, it is an eye opener.
In the last year I gained weight (10 Kg). The main reason: stopping being active and having the same diet as when I was more active. At least, is what I thought till I read about excess glucose and excessive insulin in your article.
Although I am not totally ignorant regarding the functioning of our body, I didn’t think, (better said – I ignored), about the consequences of my lifestyle.
You made me think: Time for action!
I’l start with the book you recommended, “The Diabetes Epidemic and You” by Dr. Joseph R Kraft, go thoroughly through “What Does Insulin Resistance Mean” and probably some checks.
Thank you, Jimmy! Keep us informed!
Keti
Hello Keti,
I am glad that my post was clear, easy to read and understand. Also glad that it aroused your attention.
Wow! you gained 10 Kg, due to inactivity and the same diet. I wrote a post “Lose Weight Keep It Off” please check that out on my website, it will help you. A basic tip – eat 3 times a day and fast for the rest, do not snack.
More than 3 years ago I dropped 16 Kg following a Low carb high heathy fat diet and intermittent fasting. I have put my type 2 diabetes into remission.
I suggest other books on all of my posts please check Jason Fung’s book The Diabetes Code, click the link.
Check out the videos on this post, each video is educational and eye opening.
Thanks for dropping by and commenting.
Jimmy.
Thank you for sharing your interesting article ¨What Does Insulin Resistance Mean? ¨, Diet is inextricable from the amount of healthy time we spend on Earth. Improvements in diet, as you mention in your article, are clearly associated with significant lengthening of lifespan and dramatic decreases in risk of most chronic diseases, particularly diabetes.
In this context attention to glycemic load and index is very relevant in your diet. Eating foods that have high glycemic loads is associated with greater risk of heart disease and diabetes Some people use the glycemic index (GI) which I find confusing.
For instance, watermelons have a high GI, but a typical serving of watermelon does not contain many carbohydrates, so the glycemic load of eating is low.Also, carbohydrate-selective diets are better than categorically low- carbohydrate diets, in that incorporating whole grains is associated with lower risks for cancers and better control of body weight and therefore insulin.
Hello Enrique,
Yes I absolutely agree with you inextricable time on earth is due to a nutritious healthy diet. Absolutely, the main concern for everyone living on this planet.
Type 2 diabetes and other metabolic issues are the result of insulin resistance and not the other way around, you could be insulin resistant for years, not be diagnosed with diabetes and have a heart attack or stroke.
If you have read between the lines insulin resistance = hyperinsulinemia = type 2 diabetes, according to Joseph Kraft.
I agree with you on the GI and GL, use the GL as it is a better indicator of a carb quantity. You would only eat slices of watermelon as opposed to the whole watermelon.
Limit your carbs and stop eating sugar and processed food and you will absolutely control your insulin.
Thanks for dropping by and commenting.
Thanks for sharing this article. This post is educating, informative and helpful. I don’t really know much about insulin resistance but reading your article I have a better understanding on what insulin is. You did a great job by bringing your readers to this knowledge.
What can you recommend for someone that finds it difficult to stay away from taking sugar because I am thinking a friend is at risk of having diabetes?
Hello,
I am glad that you found the article educating, informative and helpful. Insulin resistance is a hard concept to grasp because you can not see it. You may not have any symptoms for years and then boom, you have a heart attack.
On another note, yes, I agree sugar is a subject in itself. Big Sugar has made a product that is very addicting. Books have been written about sugar and quitting and the like.
I would suggest you slowly quit or stop consuming sugar cold turkey. I stopped cold turkey.
I hope this helps.
Thanks for dropping by and commenting.
Hey Jim, thanks for this wholesome information… To be frank, I was never concerned with insulin in my body until type 2 diabetes hit my Aunt and sent her to her early grave. The reality shocked every member of my family to the point that all of us now take note of what we eat. Most of my uncles that drink and smoke heavily had to stop the habit so as not to pass through the horrible torture of diabetes.
We are now more insulin-conscious in our family more than ever
Thanks for this elaborate explanation, I’m going to forward the web page to them, I know they’ll be happy knowing more tips on how to stay healthy and free from diabetes
Regards
Sammy
Hello Sammy,
I am glad that you and your family are insulin conscious. The main concern for insulin is to eat a proper nutritious diet, and control stress, get 7 – 8 hours of sleep. Other factors include not smoking, drinking and limiting medication use.
I appreciate that you will share this article with your family and friends.
Thanks for dropping by and commenting.
Thanks for this informative post on insulin resistance. This post made me understand alot about insulin resistance and has encouraged me to always check my blood glucose level with my doctor, but I would like to know if insulin resistance can be detected with blood draw and also does stress cause insulin resistance?
Hello Seun,
I would recommend you get a complete blood panel from your doctor. The only way you can detect insulin resistance is through the blood panel and you can use the HOMA-IR calculator.
Stress and sleep are major factors that affects insulin resistance, the hormone cortisol when released will trigger insulin to be released.
First and foremost get you diet and nutrition in order, cut out sugar and processed foods and then work on reducing stress levels. Try to get 7 to 8 hours of sleep every day.
Thanks for dropping by and commenting.
That was a great review. Many people are suffering of diabetes out of ignorance while some suffer it due to the fact that they can’t control what they eat They have no control over themselves. Thanks for making me understand ways to reduce insulin resistance. It’s not a big deal for one to eat natural things and reduce intake of refined carbs. Thank you.
Hello Kenechi,
Most people do not understand nutrition, and that is why they eat processed food which is loaded in sugar. Education in grade school concerning nutrition would help people understand the value of nutrition.
I agree with you it is not a big deal to eat natural whole unprocessed food, go to your grocery store, you can buy it there. You must make a lifestyle change and then get into a routine and then follow the healthy lifestyle change.
Thanks for dropping by and commenting.
Dear Jimmy,
Thanks for the post and I must say I found your post highly uplifting & educational. I can tell you I have taken some great insights from your post.
May I congratulate you on your persistence in creating this informative post. Any man who devotes that much time must of necessity make discoveries of great value to others. And you have provided great value via your post.
The history and discovery you shared are very helpful. You not only addressed the problem but the best thing is you have provided with the solution as well. I am going to implement what I learned from your post. Also, I made a note of the book by Joseph R Kraft.
You gave us an encyclopedia of knowledge via your post. To be honest one read is not enough and I am bookmarking your post for future reference. I am also going to share your post with my close friend who has Type 2 Diabetes, for sure he will find great value.
Best wishes to you, your family and your success, Warm Regards,Paul
Hello Paul,
Please take note of the other book by Dr. Jason Fung another fantastic read called The Diabetes Code.
I tried to give you as much information as I could I still have another post that will follow this post called measure IR. Coming soon.
I appreciate your sharing this article.
Thanks for dropping by and your kind words.
Hello Jim, highly researched article. From this article, I believe the issue of diabetes boils down to the choices of diet we make. To be fair on us, the generation before us were not as busy as we are today. The world is so fast today, that one barely has opportunity to eat a decent meal. Basically, I’ve really cut down my carb intake, and I eat less of this refined food. I also stay away from soda and fizzy drinks. Can you give me more practical tips to help with my daily life
Hello Louis,
I agree with you that diet and nutrition is a main factor in type 2 diabetes and any metabolic issues. Even though the generation before us were not as busy, it is relative meaning that whatever the pace was back then everyone was going at the same pace. People are eating more junk food and sugar than ever before.
Health is the most important factor in life, health is wealth and if you are not healthy how do you take care of yourself? You better have good health insurance.
Good to hear that you cut down on carbs, refined foods, and sodas.
Practical tips I would give you are quit eating sugar and try to walk for at least an hour a day. Do you want to Lose weight? Check out my other posts on my website. Watch the videos that I recommend in this post.
Thanks very much for dropping by and reading.
Hi Jimmy, great read my friend. Very interesting and quite topical for me, especially your article on intermittent fasting. This is something that I practice and I tend to fast for up to 16 hours. I started it after a friend recommended it for losing weight. I lost almost 10kg in about 3 months. I then found out about a fat diet, whereby you eat real food and basically cook everything in butter. It’s supposed to help with insulin resistance. I’m not an expert like yourself but it seems to work. Have you heard about his form of eating/fasting?
Hello Craig,
Please read the Low Carb High Fat (LCHF) diet on my website, this works in conjunction with the Intermittent Fasting. If you have lost 10 Kg in 3 months that is great. I suggest you cut down on your carbs and if you can eliminate sugar from your diet, this helps. Cutting sugar from your diet is hard to do but can be done. Do you know what your Hemoglobin A1c is? If not you need to be tested. Go to your doctor and ask for a test. Thanks for commenting. Jimmy.
Thanks Jimmy. I’ll give that a read.
Hello Craig, I appreciate you taking the time to read the articles on my site.
Thanks.
Jimmy.